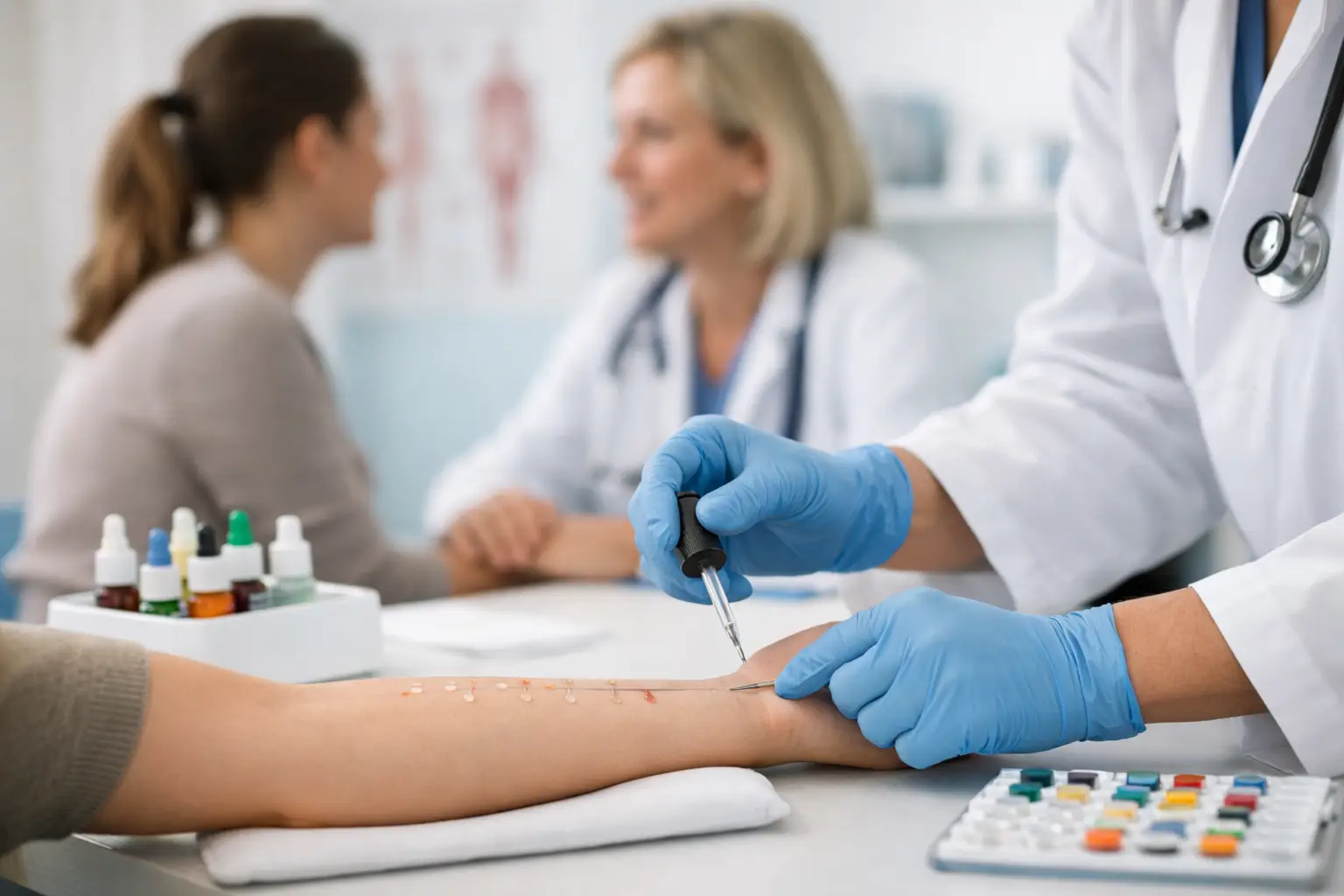
When allergies keep showing up as congestion, coughing, itchy eyes, rashes, or sinus pressure, the frustrating part is often not knowing what is actually causing them. That is where allergy testing at a primary care clinic can make a real difference. Instead of guessing whether pollen, dust, mold, pet dander, or something else is behind your symptoms, you can start with a provider who knows your overall health and can help you get answers without adding extra steps.
For many patients, the biggest benefit is convenience. If you already rely on a family medicine practice for checkups, sick visits, or ongoing care, it makes sense to ask about allergy concerns there first. A primary care team can look at the full picture, including your symptoms, your medical history, the time of year your symptoms flare up, and whether allergies may be overlapping with asthma, sinus issues, skin irritation, or recurrent infections.
Why choose allergy testing at a primary care clinic?
A lot of people assume allergy concerns automatically require a specialist. Sometimes they do, especially when symptoms are severe or unusually complex. But many allergy problems can be evaluated in a primary care setting, and that often saves time.
When testing is offered in the same office where you receive regular care, the process tends to feel simpler. You are not starting from scratch with a new provider who does not know your history. Your primary care clinician may already know which medications you have tried, whether you tend to get seasonal flare-ups, and whether your symptoms affect sleep, work, school, or exercise.
That kind of continuity matters. Allergies do not always show up in a neat, textbook way. One person may deal with morning congestion year-round. Another may have headaches and think they are getting constant colds. A child may have eczema that worsens around certain triggers. In a primary care clinic, testing is part of a broader conversation about your health rather than a stand-alone event.
What symptoms may point to allergies?
Allergies can look mild at first, which is one reason many people put off getting evaluated. They may assume symptoms are seasonal, temporary, or just part of life in South Texas. But ongoing symptoms deserve attention, especially if they keep returning.
Common signs include sneezing, runny nose, stuffy nose, itchy or watery eyes, throat irritation, pressure in the ears, coughing, wheezing, and skin reactions like hives or itching. Some patients mainly notice fatigue or trouble sleeping because nasal symptoms are worse at night. Others come in because they have repeated sinus infections and want to know whether untreated allergies are part of the problem.
It also helps to pay attention to patterns. If symptoms worsen after yard work, around pets, during weather changes, or in certain indoor environments, that can offer useful clues. Still, patterns alone do not always tell the whole story. Testing can help confirm or rule out suspected triggers.
How allergy testing works in a primary care clinic
An allergy evaluation usually starts with a conversation, not a test. Your provider will ask when symptoms started, how often they happen, what seems to trigger them, and what treatments you have already tried. They may also ask about asthma, eczema, sinus issues, family history, and your home or work environment.
From there, your clinician may recommend allergy testing if it fits your symptoms and medical history. The exact type of testing can vary by clinic and by patient need. In many cases, testing is used to identify environmental allergens such as pollen, dust mites, mold, or pet dander.
What matters most is not just getting a result on paper. It is understanding whether that result lines up with your symptoms and what to do next. A positive test does not always mean something is causing your symptoms every day, and a negative result can be just as helpful if it rules out a trigger you have been worrying about.
What to expect at your visit
Most patients want to know two things before they schedule: Will it take a long time, and will it be uncomfortable? The answer depends on the type of testing performed, but in general, the visit is designed to be manageable and straightforward.
Your provider will explain how the testing works, whether you need to stop any medications beforehand, and how results will be reviewed. This is one reason getting tested in a primary care setting can feel more approachable. You are able to ask practical questions in plain language and talk through the next step right away.
That next step may include changes at home, medication adjustments, or a broader treatment plan. If your symptoms are mild, a few targeted changes may be enough. If your symptoms are persistent or interfere with daily life, your clinician may recommend a more structured approach.
The value of in-house care
One of the strongest reasons patients look for an allergy testing primary care clinic is simple: they want answers without having to coordinate multiple offices for a common problem. When your medical team can evaluate symptoms, perform testing, and discuss treatment in one place, care becomes easier to follow.
That matters for busy parents, working adults, and older patients who do not want unnecessary delays. It also matters for children, who often do better when care feels familiar and streamlined. If a patient already comes to the same practice for annual visits, school physicals, diabetes care, immunizations, or sick appointments, keeping allergy care under the same roof can reduce stress.
Convenience should never replace good medicine, but it absolutely supports it. Patients are more likely to follow through when scheduling is easier and the process feels less fragmented.
When primary care is the right place to start
Primary care is often the best first stop for suspected allergies, especially if symptoms are new, moderate, recurring, or difficult to sort out from other everyday health concerns. Many people are not sure whether they have allergies, a lingering infection, medication side effects, or irritation from the environment. A primary care provider can help sort through those possibilities.
This is also helpful when symptoms overlap with other conditions. For example, chronic nasal congestion may be allergy-related, but it can also involve sinus inflammation, a structural issue, or irritation from dry air. Coughing may be linked to postnasal drip, asthma, reflux, or an infection. Skin symptoms may point to allergies, eczema, contact irritation, or something else entirely.
That is where a broad medical perspective helps. Instead of focusing only on one possible cause, your clinician can look at how all of your symptoms fit together.
When a specialist may still be needed
There are times when primary care testing is the right starting point, but not the final step. If someone has severe allergic reactions, complex asthma, recurring hives without a clear pattern, or symptoms that do not improve with standard treatment, referral to a specialist may be appropriate.
That is not a drawback. It is part of good care. The advantage of starting in primary care is that you can be evaluated promptly, begin treatment sooner, and get a clearer sense of whether specialist care is truly necessary. For many patients, it is. For many others, it is not.
Getting more than a test result
The real goal of allergy testing is not just identifying triggers. It is helping you feel better in daily life. That might mean sleeping through the night without congestion, getting through cedar season with fewer symptoms, helping your child stay comfortable at school, or reducing those repeated “maybe it is another cold” visits.
At a practice like Castle Hills Family Practice, patients often appreciate being able to address allergy concerns in the same place they already trust for everyday healthcare. That kind of accessible, in-office support can make it easier to move from guessing to a plan that actually works.
If allergies have been disrupting your routine, the best next step may be simpler than you think. Starting with a primary care visit can give you clarity, relief, and a care plan that fits real life.